In early September of this year (2021), our friends at Help Hope Live reached out to invite me to participate in their Spinal Cord Injury Awareness month by answering some questions that might then be featured in their newsletter.
As it turns out, they had enormous response to their request and for various (and probably very good 🙂 reasons, my replies did not make the cut.
I’m publishing them here for a closer audience who may nonetheless appreciate the reflections…
Without further ado:
HHL: Is your Help Hope Live page up to date?
It is not. (I’ve not been using that platform for content distribution, favoring instead the personal blog –
where contributors have been invited to subscribe for updates.)
HHL: Can you tell us a little bit about how your injury took place?
My injury was the result of an SUV rollover. It took place on a road trip with friends through the Arizona countryside.
HHL: What are some of the emotions and physical challenges you faced in the early days of your SCI journey?

I would categorize the “early days” of my journey as being those of the extended initial hospitalization (3 1/2 months). The physical challenges there, were largely institutional. The hospital was certainly understaffed and thus unable to care for the intensive requirements of my condition. As a result of this, I lost nearly 1/3 of my body weight (approximately 40 pounds) due to malnourishment and neglect.
In this context I was fairly far removed from friends and family. My most frequent visitor was my personal injury attorney who came about 10% for business and about 90% simply as a friend coming to share in the journey and the experience.
During that period, I was undoubtedly experiencing emotional depression, although the condition was largely unrecognized by me, or my caregivers in and of that time.
HHL: How does your life look different today than it did when you were first injured?
Viewed from the outside, my life today is a vast contrast to the early years of my injury.
My initial focus was wholeheartedly on the practice of challenging the prognosis and developing the greatest possibility of full recovery and return of function.
Additionally, we were very early in the process of understanding and developing the systems aspect of a basic home life necessary to function as a quadriplegic in my “new” physical body.
Without any “place to be” outside of bed, I remained prone or inclined for the better part of each day and each week; only venturing out of bed for the usual five days a week, roughly 6 hours a day to attend an intensive recovery therapy program at Project Walk, a cutting edge spinal cord injury rehabilitation center.
Outside of those excursions, being out of bed meant only diminished access to communications and creative work technology accessible through the laptop, and therefore just me sitting in my wheelchair with “little to do.”
Eventually, a local nonprofit foundation learned of my condition and purchased a desk on my behalf that would make a more accessible situation outside of the bedroom.
Additionally at that time, my available care consisted primarily of my brother, who lived with me, running the household in every respect in addition to ensuring I personally had all of the direct care I needed. Largely in support of him in that role, we also had about 40 hours a week of hired caregiving support, used mostly to get me up and going, out the door to recovery therapy, and back to bed when we returned in the afternoon.
In contrast, today I am running my own household, have a care team of five people* formally on payroll [*not so at time of publication due to pandemic related shortages in the overall workforce], with additional support from nearby friends in community.
I am out of bed daily, health [and care] permitting, with full knowledge of my healthcare and direct management of that as well (in the early days I knew nothing of my care needs, concerns, and the trade-offs being implicitly made.)
Really the first year was a full-time job discovering the absolute breadth of my new context – different body, different needs, different focus, different relational fluencies… Different everything.
I have since moved on in terms of my focus, having developed a much more sophisticated and nuanced appreciation of the nature and pace of “recovery,” and all of the various aspects at play, and the largest portion of my time now (after the extensive management concerns for health and care and household) is now devoted to plying my efforts in the world to better understand our shared global situation and seeking ways, large and small, to be of service in our time.
In addition to that, my own internal meditative practices have matured and hold a substantively greater role in my daily focus than they did at the time of my injury.
One frame of reference that may sum up the distinctions is a movement from Disempowered Director of my affairs, to that of an Engaged Leadership model of being.
HHL: Do you face ongoing health challenges related to your SCI? Can you give us some examples?
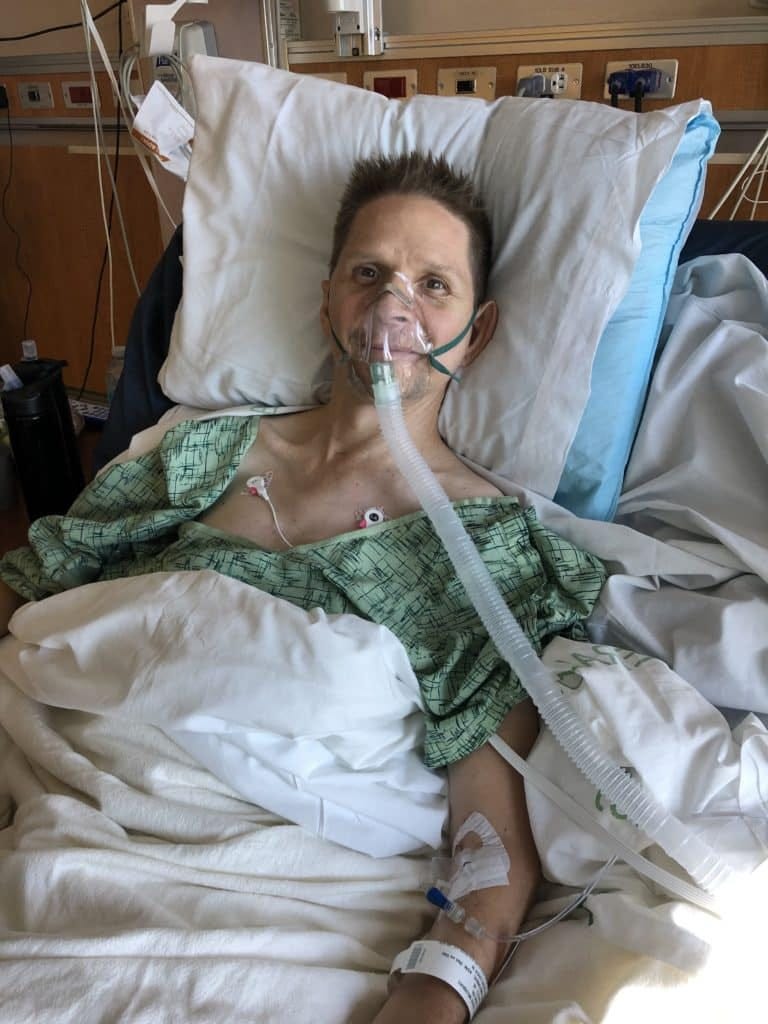
I do, and have had ongoing health challenges as a result of the onset SCI. In the earliest days these took the form of persistent skin breakdown resulting from the malnourishment and neglect in the hospital, as well as frequent urinary tract infections, again an effect of the institutional parting gift of the “superbug” bacterial infection. I literally left the hospital under IV antibiotics; a treatment regime I would revisit on multiple occasions going forward.
In the early years, many of the “health challenges” had simply to do with a lack of experience/education regarding the nature of my condition and its peripheral concerns. It was nearly a decade later that I first learned the actual specifics of the importance of proper bladder management, and the risks of death associated with its failure.
Throughout the years, with autonomic dysreflexia (A.D.) as the only information signal to indicate the presence of some infection, malfunction, or discomfort, without distinction for where in the body the source of that issue was arising, I struggled, and struggle today to keep up with ongoing and emergent issues which may range in severity from simply a shoe being too tight, to an actual life concern such as the cellulitis I contracted just last week.
Today, my most persistent concern appears to have to do with the gastrointestinal tract, though the methods available for assessment and diagnosis in that region remain a bit out of reach for someone in my condition. The recent frequency of A.D. strongly suggests some concern with motility in that region though any clarity on the matter is slowly forthcoming.
This persistent condition of full body discomfort can prove enormously distracting and in its more extreme moments can actually send me to bed where my productive capacities fall off nearly completely.
[Since this additional writing, my daily health has improved and with implementation of a few simple practices, I am optimistic for the general course of those aspects, going forward.]
HHL: When did you first begin documenting your thoughts and life on your blog? What prompted that?
There have been thus far four distinct phases of this process of reflective writing.
The first phase was simply intended as a method of sharing some window for the community of people that came forward in the acute phase of my injury and establishing a new “home life.” At this time, entries were infrequent and meant more in the capacity of a newsletter for those watching from the sidelines.
Later, my attorney, mentioned above – himself a vastly accomplished literary practitioner and connoisseur, had been for years nudging and encouraging me to write at all. Finally, in a fit of friendly exasperation, I offered to simply write 100 words a day which I would forward to him by email. He gladly, and I suspect knowingly, accepted the offer.
In short order, 100 words became 1000 words, and a trivia of reflection blossomed into an ongoing narrative of my daily life. These writings were not published*, and while not strictly daily, became a regular part of my personal practice.
These “Letters to Charles,” were written frequently in the years between 2012 and 2014.
This process was, as much as anything, about engaging with a willing mentor to help shape and refine my capacity with the craft.
In researching my reflection for this question, I stumbled across a number of other instances of writing that I had published and forgotten about. I guess the best answer to this question is really that I have always been a writer. It comes out in different ways over the years. The effort of writing every day for the year of 2020, was just a spontaneous inspiration focus on practice and to narrate what promised to be a substantial year in my life. (Health, robustness of care stability of home, and access to finances, were all clearly uprooting from their prior conditions of reliability, little did I know, what indeed was in-store, not just for me but for the world as well.)
HHL: When did you begin your work on MettaCare?
The “When” of MettaCare is a question that can be answered in many ways. Like my comment about writing, above, the subject is, and in fact has been, long a part of me. The “lovingkindness” of care, the omnidirectional awareness that gives it real power and real ground, is a practice that ultimately emerges as an embodied way of being.
How many years ago did it become important to me to practice and become each moment more skillful, more wise, or more intentional with care?
Indeed, this naming of the construct emerged in dialogue, first with my close friend David, and shortly after, with my daughter, and our extended community of care partners and friends.
When did this work begin to manifest itself in David, who had directly engaged in hospice care with two of our seniors, now deceased ancestors?
The dialogic construct became part of our lives and work, probably beginning in 2012 or 2013. The term itself would emerge in formal meetings with our extended care partners in late 2014 and early 2015 when the mode shifted from early “sensing” of the distinct body of work, towards a more active inquiry into its nature and possibilities.
HHL: Can you expand on the idea (from your video on MettaCare) that it’s not just about getting out of bed with assistance, but about finding a connection with the reason WHY you want to get out of bed to begin with?
The act of care is fundamentally a movement of service. At the very least, if I experience an emotion of care for some subject apparently outside of my field of influence, I am in service by expanding the field of awareness around that suffering.
Fields of awareness are the essential source of action.

When my care is truly oriented to that subject of service (and not simply some reactive and subconscious care for my own suffering as anxiety or loneliness — itself a valid subject of care), I am seeking to nurture that “other” for the depths of their essential expression of being.
As Simon Sinek would put it, what is their “Why?” Is it simply to live?
Research has shown that when a person has a sense of Purpose in their life, a vast range of markers for well-being go up in their expressions of fullness. Purpose, “Why,” can be a profound aspect of our life’s journey, growing, touching others, increasing the depths of our appreciation, love, and compassion.
In what I imagine a MettaCare context to be, an individual is not simply coming to service the dead weight of my flesh, but to participate with the fundamental intention to diminish the harm that I do, and to increase the well-being that I offer, and that I seek to nurture in the world at large.
Caregiving for me as a patient, is not just caregiving in the industrial sense of taking away gross suffering and increasing physical independence, but rather the participation in a larger vision of life.
Likewise, and reciprocally, I meet those who come into my field as subjects to my inherent sense and value of caring, loving kindness, and being of service. Again, to what?
As a caregiver (partner in care) moves into my field, what is it for them, at their greatest depths, that they long to serve/to become/to experience? To the degree that they can realize their own sense of purpose with clarity, joyfulness, and with intentionality, is that to which I can reciprocate the flow and liveliness of care that moves through the field of awareness that we co-create.
HHL: How does the idea of “community” play a role in and help fuel your work with MettaCare?
As you can see above, care itself is implicitly an act of community. Care is not an object, but a relationship moving between two or more “others.”
Intention, service, well-being, all emerge in context. What is the level of maturity within a given community to cultivate the field of awareness such that it is filled with care? Care and neglect can perhaps be reframed as polarities, maybe, freedom and embrace…
MettaCare is at its essence an intention to nurture our global community, it’s constituent communities, and ourselves into a greater maturity of care, one that I think is plainly obvious in its necessity if we are to meet our current evolutionary challenges.

MettaCare does not exist without community, and at the rate things are going, our communities will be increasingly challenged to exist without some expression of MettaCare.
I want to be careful here, MettaCare is not some ideology, the name, its identification with me or these writings, or the practices I aspire to perfect, can all fall away — it is the essence of care that must blossom and bloom to a much greater degree if that we know as community is to flourish in these times.
HHL: Do you feel that people can easily mistake a spinal cord injury or disability for someone’s entire identity? Can that perspective be harmful?
It is in our nature, perhaps in the nature of mind itself, to make models of that which is before us, to make models of ourselves, to simplify the vast complexity of the mystery, and then relate to that, those objects, those constructed models, rather than the actual enormity, indeed the infinite eternity of what is truly present.

The grossness of a durable appendage such as a wheelchair, is not much unlike skin color, or levels of attractiveness, or any other outward display which we may take as visual cues for how we are to relate to this “other.”
For any of us, the degree to which we revert to relating to any part of our experience as the model, rather than remaining vulnerable to the profoundly unpredictable and mysterious reality, both creates a sense of continuity, security, clarity, and safety, while simultaneously walling us off from the real wealth of opportunity presenting itself in all of its novel glory.
Any perspective can be harmful; it all comes back to care. What am I learning about this which is before me? How much am I attempting to constrain for my own benefit? How may I be of service, both to this other, and to myself in this moment?
HHL: What are some of the ongoing costs that you fundraise for? Specific dollar amounts are great if you have any examples.
The question of fundraising is, for me, not so cut and dried. I am raising, if I am, as much community, as much relationship, as finance. Who is that audience? What is our relationship? What community are we enacting?
Each month I am responsible for some part of the livelihood of a small band of individuals who devote a portion of their life energy, not just to my own care, but also to developing the resources they need for theirs (inclusive of their own extended fields of care.)
So, in plain terms, I have a monthly expense of about $12,500 for “caregivers” who come to aid me in the physical aspects of life. Sadly, this number represents a truly poor wage to account for that service. It is nonetheless, what I currently afford. Truly that number should probably be half again as much. ($15,000+/month)
In contrast to that, ongoing expenses seem relatively trivial. I probably use an additional $400 per month in medical supplies; an additional average of probably $300 a month for doctors and other specifically medical services; as well as another $150 per month for prescribed nutrient supplementation to help me maintain a basic foundation of material health with which to meet the ongoing pressures on that aspect of my well-being.
Of course, there is the occasional expense for durable medical equipment, $3000 for a bathroom chair here, $5000 for a wheelchair there, and “nickels and dimes” along the way to manage other accessibility concerns.

Beyond this, when finance of any kind is going well, I will quickly spend an additional $500-$1500 monthly for active therapeutic support, both for physical exercise, as well as the development of a more robust physiological health foundation.
Even under the weight of financial stress, my life is a source of gratitude and well-being. That said, the expenses noted above just about get me to zero, meaning healthy, mobile, and free enough of distraction to focus on a more familiar generosity. This fundraising is about a foundation.
I am deeply saddened by how little of this resource such a great number of others do not enjoy and, in fact, are set so far apart from. For years I provided much of this for myself and the community around me from the proceeds stemming from the liability in my initial injury. The last few years have brought me much more face-to-face with this hard and tragic reality.
HHL: How does covering these costs improve your day-to-day life or your health?
The difference between the absence and presence of the aforementioned foundation cannot be overstated.
Without this foundation secured, the best-case scenario is the life of a rote business manager, not as an occupation or career, but as an entire way of life – every moment spent “holding together” the bottom line. There is of course profit in this business of life, that must be sought again and again within. Accomplishing each day brings the rewards of a sense of gratitude. Staying well for one more week, another source of inspiration and joy.
Of course, that slides away quickly if the manager cannot uphold the income and managerial effort necessary just to keep things moving, and things get very dark indeed.
With these fundamental costs covered, the sky begins to open up, with it, the heart lifts more freely, and the well-being of the body follows quickly behind. To be certain, money and care, stability of household, these are not guarantees of well-being or physical health, but they do provide a source of power that can be leveraged effectively in that direction.
HHL: How has fundraising with Help Hope Live helped you since your injury?
Fundraising with Help Hope Live has been a lifesaver, FULL STOP.
In the earliest days of my relationship with the organization, it was helpful, one more piece coming into place in support of a full mandala of understanding my new condition.
More recently, and just before the pandemic, when things for me looked as bleak as they had ever appeared, the relationship with HHL appeared as a cornerstone of possibility.
During a year in which I miraculously survived at an expense of over $200,000, the roughly $50,000 raised on my behalf through the campaign magically made All the difference in the world. I cannot conceive of where I would have been without it.
HHL: What advice would you give to a newly-injured individual or family?
The advice for newly injured individuals or family, is a constant and challenging question.
Depending on the severity of injury – and sometimes to a lesser extent than we might think – the impact of this moment cannot be overstated.
How can we, any of us, imagine how to pick out the important signals in the cacophony of noise that makes up this profoundly unsettling new context of life, and even “self,” for some; let alone, how could we know what to say?
“Take it slow.”
“Listen closely.”
“Feel deeply.”
“Consider carefully.”
“Learn; think ahead; nurture your relationships; care for yourself and your community…”
In my experience, most people in the situation are listening frantically. A deluge of information, from formal/official, and informal and unofficial sources, is pouring in from every direction. Some of the professional information is good; sadly, some of it is not so good. Much of the informal information is well-meaning, some of it is profoundly important, some of it is dangerous. How to know the difference?
I think in response to this inquiry, the advice goes not so much to the newly injured individual, or their family, but rather to those of us who are, and hopefully will remain their community.
Catastrophic injury is a rebirth of sorts. So much will change, it is not unfair to call it “everything.” As in the case of any birth, it is the community around that makes all the difference in the world.
Just as we would for a new mother, a new father, a new infant, we hold space. We take it slow. We listen carefully, we feel deeply both the joys and the concerns, we consider carefully our service to this emerging dynamic of the family. We drink in the nutrient of this new moment, letting it nourish and change us so that we may be stronger, so that we may be more wise, and our service more integrated to the well-being of our community.
HHL: What does hope mean to you?
Hope. Hope is an emotion, it is a longing for something. In essence hope fills our field of awareness, hope is a prayer.
The Sufis say, “when the guest is being longed for, it is the intensity of the longing that does all the work.”
Hope is the emotion into which we pour our intention. What is our purpose? What is our why? At our very best, what is it we long to see in ourselves, in the world around us, and those we love?
The Sufis go on… “Look at me, you will see a slave to that intensity.”
HHL: What would you like to add that we have not asked about?
Thank you for asking. 🙂











Thank you for sharing more about the transformative experiences of your life. This piece inspires and provides context for our appreciation of who you truly are!